Market leader for minimally invasive, image-guided laser ablation systems, Monteris Medical, has announced today that results from a multicenter clinical study of its NeuroBlate® System have been published in the peer-reviewed journal Neurosurgery. Authored by physicians at 14 leading academic medical centers, the prospective study involving 223 brain tumor patients is the largest of its kind detailing beneficial results following minimally invasive laser interstitial thermal therapy (LITT).
“Overall survival was 73% at 12 months, which was better than anticipated for this patient population with severe disease, high rates of baseline comorbidities and an extensive history of previous treatments,” commented Dr. Eric C. Leuthardt of Washington University School of Medicine in St. Louis, Mo., and the study’s principal investigator. “In addition, patients who had LITT also experienced improvements in quality of life that positively impacted their emotional health and ability to perform daily activities.”
The study found that “in the appropriate use scenarios, [LITT] can achieve a similar extent of resection to craniotomy with lower risk of complications.” Important patient and healthcare economic measures such as length of stay, ICU time, discharge to home, and readmission rates were also favorable to those reported in the literature for craniotomy. Most of the patients in the study had glioblastomas or metastatic brain tumors. Data included in the Neurosurgery publication comes from the LAANTERN Study (NCT02392078), an ongoing multicenter prospective registry collecting real-world outcomes and quality of life data using the NeuroBlate surgical tool. The 500th patient was recently enrolled in LAANTERN and the company expects to enroll and follow at least 1,000 patients during the course of the study.
“We are pleased with the positive patient and health system impact of NeuroBlate technology as documented in this study,” said Martin J. Emerson, president and chief executive officer of Monteris Medical, the maker of the NeuroBlate System. “We believe these data will continue to help physicians identify the appropriate surgical tool for their patients. Four years ago we made the commitment to gathering real-world evidence on NeuroBlate, and now LAANTERN is starting to produce meaningful outcomes data. As we enroll more patients, insights for physicians will become even richer.”
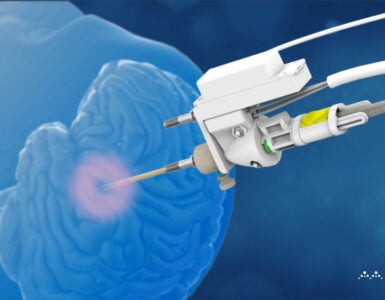
The NeuroBlate System utilizes robotically controlled laser thermal therapy that directs an MRI-guided laser to ablate unwanted tissue in the brain where the lesion, or abnormal tissue, originates. Unlike traditional brain surgery, a procedure with the NeuroBlate System does not require a large opening in the skull. Instead, surgeons create a small hole in the skull, about the diameter of a pencil. While the patient is in the MRI machine, the doctor guides a small laser device (probe) through the hole and into the lesion. The precise nature of the procedure helps to lessen the likelihood of harm to nearby healthy brain tissue.
To date, nearly 3,000 procedures have been performed with the NeuroBlate System at more than 80 hospitals in the U.S. and Canada.