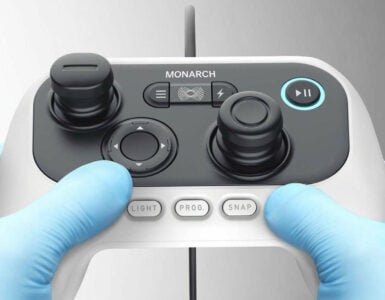
Ethicon*, part of the Johnson & Johnson Medical Devices Companies**, today announced the results of a new real-world study that shows its ECHELON CIRCULAR Powered Stapler was associated with a 74% reduction in anastomotic leak rates (1.8% vs. 6.9%)1 and a 44% reduction in 30-day inpatient hospital readmission rates (6.1% vs.10.8%) after colorectal surgery compared with manual circular staplers.2
The study, published in Surgical Endoscopy, shows the groundbreaking device is just as effective in reducing life-threatening and costly surgical complications in real-world surgical practice as demonstrated in recent clinical studies, where the leak rate was 1.7% for the ECHELON CIRCULAR and as high as 11.8% for manual staplers. For the real-world study, investigators drew from data in the ECHELON CIRCULAR clinical trial (165 patients) and the Premier Healthcare database (1,348 manual circular patients) for a matching adjusted indirect comparison of patients who underwent left-sided colorectal resection.3
“The data is very positive in terms of postoperative complications and intraoperative events and ease of use, specifically related to the deployment of the circular powered stapler,” said study co-author Patricia Sylla, MD***, a colorectal surgeon and Associate Professor of Surgery at Mount Sinai Hospital in New York. “While anastomotic leaks are a complex problem with various contributing factors, the results of this study highlight the important role that the surgical stapler can play to reduce the potential for complications in colorectal surgery.”
Each year, more than 600,000 colorectal surgical procedures are performed in the United States4 and despite advances in surgical technique, the incidence of anastomotic leaks remains high, occurring in nearly 12% of colorectal procedures.5
“The reductions in anastomotic leaks associated with the ECHELON CIRCULAR are so profound, not only in this study, but in previous ones, a closer look at stapler selection for colorectal surgery is warranted. It could lead to a change in standard surgical practice and improved patient outcomes,” said Ron Landmann, MD,*** FASCRS, Section Chief of Colon and Rectal Surgery at Baptist MD Anderson Cancer Center in Jacksonville, FL, who was not involved in the study.
An anastomosis is a critical part of colorectal surgery in which two ends of the colon are connected with staples after part of the organ has been resected or removed due to damage or disease. If this connection is faulty or weak, an anastomotic leak may occur, which can lead to lengthier hospitalization, increased healthcare costs, and/or death.6,7 Studies show the mortality rate associated with anastomotic leaks can range from 10% to 15%.8 The risk of death can be 3- to 15-times greater if an anastomotic leak is present.9,10 ,11,12
The ECHELON CIRCULAR combines two innovative and proprietary technologies — 3D Stapling Technology that evenly distributes compression13 and Gripping Surface Technology (GST) for gentler handling that reduces compressive forces on tissues.14 ECHELON CIRCULAR significantly reduced leaks at the staple line without compromising perfusion.15
“The results of this study well exceeded our expectations and deserve strong consideration by the surgical community,” said Sanjoy Roy, Senior Director, Global Health Economics and Market Access, Ethicon, Inc. and a co-author of the latest real-world study. “The evidence, along with the innovation in design and performance, supports the possibility of this device raising the standard of care in the hands of surgeons.”
ECHELON CIRCULAR is the latest addition to a clinical and real-world evidence program that includes the publication of nine peer-reviewed studies in seven countries spanning more than 60 authors and more than 46,000 patients. ECHELON Powered Staplers are the only brand of staplers back by large-scale real-world evidence in bariatric, colorectal and thoracic surgery. Click here to learn more about ECHELON CIRCULAR.
*Ethicon represents the products and services of Ethicon, Inc., Ethicon Endo-Surgery, LLC and certain of their affiliates. All other trademarks are the property of their respective owners.
**The Johnson & Johnson Medical Devices Companies comprise the surgery, orthopaedics, vision and interventional solutions businesses within Johnson & Johnson’s Medical Devices segment.
***Consultant to Ethicon
- A retrospective matched analysis of 165 Echelon Circular cases from clinical study, and 1,348 manual circular stapler cases from Premier Healthcare Database [ECHELON CIRCULAR 1.8% (3/165) vs. manual circular 6.9% (93/1348), p<0.001]
- A retrospective matched analysis of 165 Echelon Circular cases from clinical study, and 1,348 manual circular stapler cases from Premier Healthcare Database [ECHELON CIRCULAR 6.1% (10/165) vs. manual circular 10.8% (146/1348), p=0.019]
- Pla‐Martí, V., Martín Arévalo, J., Moro‐Valdezate, D. et al. Impact of the novel powered circular stapler on risk of anastomotic leakage in colorectal anastomosis: a propensity score matched study. Tech Coloproctol (2020). doi.org
- sages.org
- Truven Commercial and Medicare, USA Colorectal Complication Rates 2010-2015
- Trencheva K, Morrissey K, Wells M, et al. Identifying Important Predictors for Anastomotic Leak After Colon and Rectal Resection. Annals of Surgery. 2013; 257: 108.
- Schiff A, Brady BL, Ghosh SK, et al. Estimated Rate of Post-Operative Anastomotic Leak Following Colorectal Resection Surgery: A Systematic Review. Journal of Surgery and Surgical Research. 2016;2(1): 060-067.
- Hyman, Neil MD; Manchester, Thomas L. MD; Osler, Turner MD; Burns, Betsy NP; Cataldo, Peter A. MD; Annals of Surgery: February 2007 – Volume 245 – Issue 2 – p 254-258 doi: 10.1097/01.sla.0000225083.27182.85
- Ribeiro et al. 2019 (Brazil) – The largest impact of AL was on the mortality rate, which was found to be 13.49 times higher in AL patients than in patients without AL in the analysis adjusted for age, gender, cancer diagnosis, and timing of surgery (p < 0 001).
- Gessler et al. 2017 (Sweden) – Thirty day mortality was 5% in the leakage group compared to 0.6% in the none leakage group (p 0.015). Similarly, the 90-day mortality was higher, 8.3 vs. 2% (p 0.004).
- Popescu et al. 2017 (Romania) – The mortality rate in patients with AL was significantly higher compared to the no leak group 28.6% vs. 1.9% (p<0.0001).
- Turrentine et al. 2015 (US) – Unadjusted analyses revealed significant differences between patients who had anastomotic leaks develop and those who did not: morbidity (98.0% vs. 28.4%; p < 0.0001), length of stay (13 vs. 5 days; p ≤ 0.0001), 30-day mortality (8.4% vs. 2.5%; p < 0.0001), long-term mortality (36.4% vs. 20.0%; p ≤ 0.0001), and hospital costs (chi-square [2] = 359.8; p < 0.0001).pubmed.ncbi.nlm.nih.gov
- Staple line analysis in benchtop testing, comparing Ethicon CDH25P to Medtronic EEA2535.
- Benchtop testing on porcine colon, comparing Ethicon CDH29P to Medtronic EEA2835, p<0.001.
- Benchtop testing in porcine tissue ≤30mmHg (26mmHg average pressure experienced during intra-operative leak test), comparing Ethicon CDH29P to Medtronic EEA2835 (p<0.001) and preclinical perfusion model, in which perfusion was not significantly different between devices.