The advancements in telecommunication and robotic surgery have made the concept of telesurgery a promising and feasible option to leverage technology for better access to better surgical care. The end vision may be what is considered remote surgery, whereby a surgeon can operate on a patient from a distance, creating a process to minimize travel, deliver care to underserved populations, address the impending surgeon shortage, and decrease the risk of infections, to name a few. But telesurgery today has progressed to the beginning of an exciting new chapter called Performance-Guided Surgery with the convergence of augmented intelligence and machine learning to provide a true digital surgical assistant for the first time.
Asensus Surgical is leading the charge by digitizing the interface between the surgeon and the patient to unlock new capabilities with a robotic-assisted platform to perceive (computer vision), learn (machine learning), and assist (clinical intelligence) in surgery. The intended outcome: to enable consistently superior outcomes by guiding improved decision making, enriched collaboration, and enhanced predictability for all surgeons—independent of skill level and experience.
In this article, Anthony Fernando, President & CEO at Asensus Surgical, provides his thoughts and predictions for the future of robotic telesurgery.
What are the biggest challenges that need to be overcome for telesurgery to be a reality?
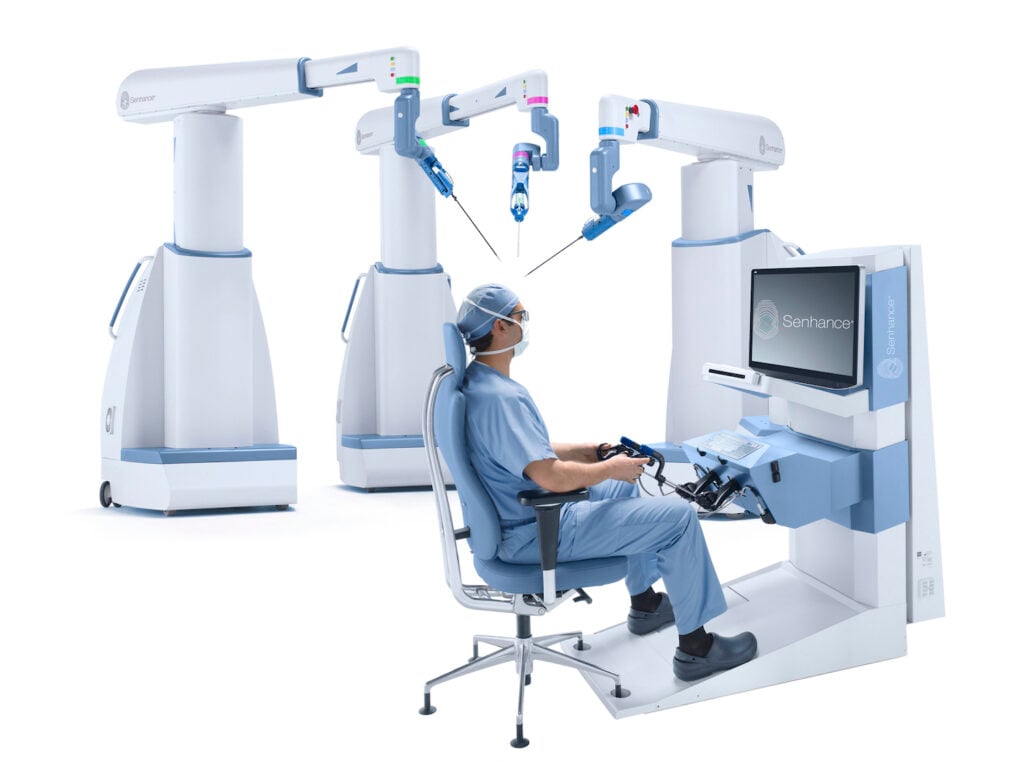
Anthony Fernando: Like any emerging technology or protocol, there are going to be visions of its global or market impact, as well as the need to address challenges and hurdles to achieve global scale. On the simplest level, telesurgery is an emerging application that utilizes wireless networking and robotic technology. To ensure the success of telesurgery, the interface between the surgeon and the patient needs to be digitized. The digital transformation trend, or the move towards the Internet of Medical Things (IoMT) – which is described by Deloitte as the growing connected infrastructure of medical devices, software applications, and health systems and services able to generate, collect, analyze, or transmit health data or images to facilitate streamlined workflows, more accurate diagnoses, fewer mistakes, and lower costs of care – will ensure patients get better treatment with the implementation of virtual reality tools, wearable medical devices, telehealth, and even telesurgery. Asensus Surgical’s Senhance® Surgical System with its Intelligent Sugical UnitTM (ISUTM) is making meaningful progress on the telesurgery front. For instance, the ISU is the world’s first and only augmented intelligence-and machine vision-capable surgical system approved by the FDA and has the capability to recognize anatomy, leverage image analytics for the first 3D virtual measurement capability in surgery and harness the power of a virtual assistant to enhance the surgeon’s ability to use information from the surgical field in real-time.
The Senhance System technology is currently available for use in a broad range of laparoscopic procedures, which account for 50% of all surgeries, however, the proliferation of 5G will be the key to bringing remote surgery to reality. The 5G network is not currently mature enough to support the bandwidth needed to successfully and safely perform remote surgery. For instance, latency is an issue. Consider the implications of lag time during surgery if the network slows or buffers during a procedure. You need the combination of 5G network, low latency, and a fast data connection to enable telepresence in real time and allow surgeons to effectively operate on the patient as if they were in the same room. Surgeons need to have complete confidence in their network capabilities to achieve the potential benefits remote surgery holds.
How do you think telesurgery will work in the short, medium and long-term?
Anthony Fernando: The original vision behind robotic-assisted surgery stemmed from the Department of Defense’s need to decrease battlefield casualties and provide expert remote surgical care immediately after major trauma occurs. However, when surgical robotics was initially introduced in the 1990s, the value was in the form of minimizing incisions and therefore trauma in patients. The surgeon was working remotely for the first time—yet just a few feet away from the patient in the same OR.
As telesurgery has evolved with the digitization of the interface between the surgeon and the patient and the addition of augmented intelligence and machine learning to robotics, telesurgery today—which is more commonly known as Digital Laparoscopy—is dramatically improving critical decision making, driving predictability, and helping level-the-field by gathering, analyzing, and presenting rich information and insights to empower surgeons of all levels of experience with deeper situational knowledge. Surgeons can now operate with familiar laparoscopic motion in a relaxed sitting position, an eye tracker to allow them to control the camera for the first time simply using eye movements, haptic force feedback for an increased level of security, a digital fulcrum to create a dynamic virtual pivot point that helps minimize the incision trauma and limit forces applied on the patient, and robotic 3mm instruments to further reduce the invasiveness of surgery. The net impact of Digital Laparoscopy is a pathway to advanced surgeon training, enhanced surgical collaboration, and increased efficiency.
As we begin to see more widespread adoption, I believe the next phase of telesurgery will initially occur inside of a hospital where there is one surgeon sitting in one room performing two or three surgeries in different operating rooms in parallel with support staff in each room to assist the surgeon. In time, this scenario could be rolled out hospital system-wide and then eventually could expand to surgeons performing telesurgery in different cities, states, and facilities around the world.
In the future, large-scale adoption of remote telesurgery could revolutionize healthcare and surgical treatments around the globe — especially in small hospitals and developing areas that don’t have as much access to top-notch healthcare. Coupled with 5G, telesurgery could provide invaluable assistance, allowing procedures to be performed less invasively, reducing complications, and expediting access to critical care.
What types of procedures are best suited to telesurgery?
Anthony Fernando: Digital Laparoscopy integrates additional technological advances beyond robotics to help surgery become more instinctive, more responsive, and more focused. In return, this creates an environment for surgeons that is more conducive to perform a greater variety of procedures, reach more patients in more care settings, and lessen the physical toll on surgeons. My assumption would be that initially, remote telesurgery would be conducive for the same procedures we are using Digital Laparoscopy to address today with the Senhance System, which are soft-tissue procedures such as General, Bariatric, Colorectal, and Gynecologic surgeries.
What benefits would telesurgery provide to patients and hospitals?
Anthony Fernando: Not unlike Performance-Guided Surgery, the immediate benefits of remote telesurgery will be centered around three core areas: outcome consistency, access, and efficiency.
Healthcare delivery in surgery is variable in procedural efficiency, surgical skill, and patient outcomes. There is a lack of standardization in these areas, which increases healthcare costs and directly impacts patient safety, recovery success, and time. This can result potentially in repeat surgery and additional medical treatment which is costly to the healthcare system. In fact, today one in five surgeries result in one or more complications.
Most immediately, Digital Laparoscopic technology with augmented intelligence can address surgical variability and outcome consistency by providing real-time guidance and reducing the physical and cognitive burden on surgeons that can lead to burnout and mistakes. With machine learning, surgeons can review surgical data and iterate procedures to improve outcomes.
With the implementation of a more robust and widespread 5G network, remote telesurgery opens the door to more effective care and surgical treatment in underserved countries, giving populations that have limited access to care and advanced surgical expertise the ability to receive much-needed surgery from a surgeon sitting remotely. The AMA also predicts a surgeon shortage on the horizon, so the ability to treat more patients with fewer surgeon resources will be a key need.
Lastly, telesurgery will allow for more efficiency. Surgeons and hospitals will have the technology needed to perform procedures in multiple rooms, simultaneously. With the support of in-room surgical teams, the surgeon will not have the downtime of transitioning from one room to the next. Eventually that could be physically expanded to other geographies.
What critical technologies are needed for telesurgery to advance?
Anthony Fernando: Technology will drive the future of telesurgery both on the network infrastructure side, which we have discussed, but also on the robotic-assisted surgery side. The digital transformation means that we move beyond what has become the standard in robotic surgery and look to the future—a new era of Performance-Guided Surgery which refers to the next-level technology that completely changes the idea of what’s possible in surgery.
At Asensus, our focus is on digitizing the interface between the surgeon and patient to pioneer a new standard of surgery for increased control, less variability, and consistently superior outcomes. When you add machine vision, augmented intelligence, and deep learning capabilities to robotics, you can improve decision making, provide enriched collaboration, and enhance procedure predictability. The impact: the best possible patient outcomes independent of surgeon skill level, training, and experience. This transition of thinking and innovation is what will drive the larger digital transformation needed to enable the future of telesurgery and other future surgical improvements that we have not even imagined yet.
Something else that is allowing Asensus to move towards telesurgery is the new telemonitoring platform called Senhance Connect. Senhance Connect allows surgical peers from around the world to remotely observe a surgical case being conducted on Asensus’ Senhance Surgical System via cameras and communicate with an expert surgeon about the most advantageous practices. Bringing surgical peers together through a connected interface became increasingly important during the COVID-19 pandemic and serves as a proof of concept of sorts for the future of telesurgery.