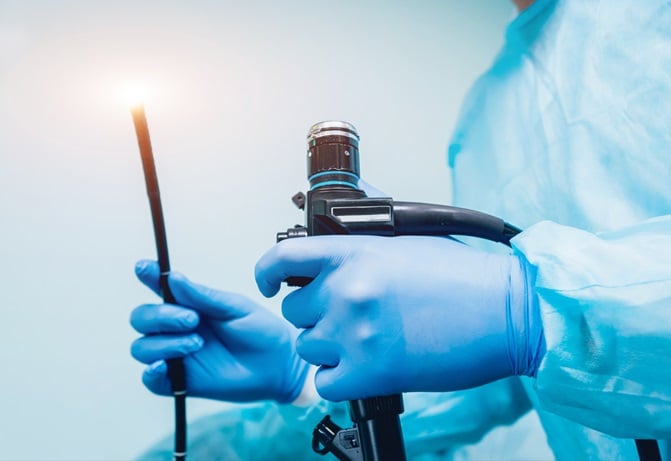
Overview
This paper explains how commonly used materials to make lenses for endoscopes likely lead to poor performance due to the performance limitations of the chosen materials. The reprocessing of endoscopes and the associated costs should be areas of concern or those looking to mitigate contamination issues along with enabling an optimized cost of ownership. We will review the capability of synthetic sapphire in endoscopic applications and how it is often a better choice than conventionally used lens materials.
Synthetic sapphire is a highly valuable material in various medical applications due to its exceptional properties. Sapphire is a form of crystalline aluminum oxide (Al2O3) and is produced in laboratories rather than being mined from natural sources. It possesses several characteristics that make it ideal for medical use. A comprehensive review of the various types of synthetic sapphire and properties can be found here.
Problems in Endoscopy
One of the largest complications with camera-guided endoscopes is avoiding the buildup of blood and other bodily fluids around the camera lens, which can often obstruct the view during many critical procedures. Endoscope materials have to endure multiple procedures, but also the standard sterilization procedures that endoscopes go through between uses.
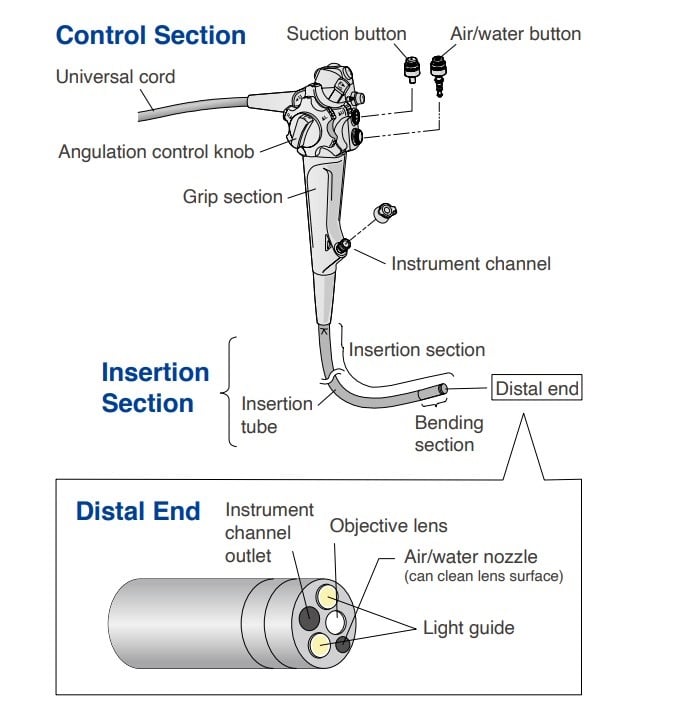
The endoscope has three parts: the control section, the insertion section, and the connector section. The insertion section of the endoscope contains the distal tip.
The objective lens is typically a super-wide-angle lens in order to visualize a large area of tissue at one time. In order to view tumor tissue in a more detailed manner, some endoscopes have an optical zoom feature. They also support high-definition video displays. Light guide fiber bundles conduct light from the external light source through the endoscope to illuminate body cavities. Endotherapy devices are pushed in and out of the instrument channel for harvesting tissue (biopsy), removing tumors, cauterizing bleeding lesions, etc. The nozzle on the distal tip is used to clean the lens with water and expand body cavities by insufflating them with air.
Sterilization of endoscopes is a critical step to prevent the transmission of infections between patients and maintain patient safety during medical procedures. The sterilization process for endoscopes involves several key steps and must adhere to strict guidelines to ensure that the instruments are free of microorganisms, including bacteria, viruses, and spores.
Several sterilization methods may be used for endoscopes, including the following:
- High-Level Disinfection (HLD): High-level disinfection is the most common method for sterilizing endoscopes. It involves immersing the endoscope in a high-level disinfectant solution for a specified period, typically following the manufacturer’s instructions. This process kills a broad spectrum of microorganisms, including bacteria, viruses, and fungi.
- Sterilization by Steam (Autoclaving): Some endoscope components, such as those made of metal or heat-resistant materials, can be sterilized using autoclaving. The endoscope is placed in a sealed autoclave chamber, and high-pressure steam is used to achieve sterilization. Steam sterilization is typically not suitable for the entire endoscope due to its sensitivity to heat.
- Ethylene Oxide (EtO) Sterilization: Ethylene oxide gas is used to sterilize heat-sensitive endoscope components and accessories. The endoscope is sealed in a gas-permeable bag, and EtO gas is introduced to kill microorganisms. This method is typically used for items that cannot withstand heat or moisture.
- Hydrogen Peroxide Gas Plasma Sterilization: Hydrogen peroxide gas plasma is used for sterilizing heat-sensitive endoscope components. It works by generating a low-temperature plasma that breaks down hydrogen peroxide into reactive radicals, effectively sterilizing the surfaces of the endoscope components.
Endoscope lenses are typically made from specialized optical materials that are chosen for their optical clarity, durability, and resistance to harsh environmental conditions. The choice of materials is critical to ensure that endoscope lenses can provide clear and distortion-free images during medical procedures. Some of the common materials used for endoscope lenses include:
- Glass: Traditional endoscope lenses are often made from high-quality optical glass. Borosilicate glass, fused silica, and other optical glasses are chosen for their excellent optical properties, including low dispersion and high transmittance in the visible and near-infrared (NIR) spectra.
- Sapphire: Synthetic sapphire lenses are valued for their exceptional hardness and scratch resistance. Sapphire is used in applications where the lens may come into contact with abrasive or sharp objects, as it can withstand wear and tear better than glass.
- Plastic: Acrylic, Polycarbonate, and Others: In some cases, especially in disposable or lower-cost endoscopes, plastic lenses are used. Acrylic and polycarbonate are commonly chosen plastics due to their optical clarity and lightweight properties. However, plastic lenses may not offer the same level of optical quality as glass or sapphire.
- Fused Quartz: Fused quartz, similar to fused silica, is used in high-temperature applications or when resistance to thermal shock is required. It is highly transparent in the ultraviolet (UV) and visible spectra.
- Calcium Fluoride (CaF2): Calcium fluoride lenses are used in some specialized endoscope applications, particularly when operating in the ultraviolet (UV) range. CaF2 has excellent UV transmittance but may not be as widely used as other materials.
The choice of lens material depends on the specific requirements of the endoscope, including its intended use, optical performance, and durability. For example, rigid endoscopes used for general surgery may use glass lenses, while smaller, more flexible endoscopes used for procedures like colonoscopies might use plastic lenses.
In addition to the lens material, endoscope lenses are typically coated with anti-reflective coatings to minimize glare and reflections and enhance image quality. These coatings are designed to improve light transmission and reduce unwanted optical artifacts.
It’s important to note that advances in lens manufacturing technology and materials continue to drive improvements in endoscope performance, allowing for better image quality, reduced distortion, and increased durability, ultimately benefiting both medical professionals and patients during diagnostic and surgical procedures.
Polycarbonate is a common material used in various medical devices and equipment, including certain components of endoscopes. While polycarbonate is durable and can withstand a range of conditions, including exposure to chemicals and heat, it can experience failure modes during sterilization processes, especially when exposed to conditions that exceed its limits. Some failure modes of polycarbonate during sterilization include:
- Thermal Deformation: Polycarbonate has a relatively low heat resistance compared to some other materials. During sterilization processes that involve high temperatures, such as autoclaving (steam sterilization), prolonged exposure to elevated temperatures can cause polycarbonate to soften and deform. This can result in distortion, warping, or even structural failure of polycarbonate components. See figure #1
- Cracking and Crazing: Exposure to certain sterilization methods, particularly those using harsh chemicals or conditions, can lead to the development of cracks, crazes, or stress fractures in polycarbonate surfaces. For example, exposure to strong oxidizing agents or acidic solutions may degrade the material and lead to visible damage. See figure #2
- Chemical Degradation: Polycarbonate is susceptible to chemical degradation when exposed to certain sterilization chemicals or agents. Harsh chemicals, such as strong acids or bases, can break down the polymer chains of polycarbonate, leading to a loss of material integrity and mechanical properties.
- Discoloration: Polycarbonate may undergo discoloration or yellowing when exposed to high temperatures or specific chemicals during sterilization. While this may not always indicate structural failure, it can affect the aesthetics of the material and potentially impact its transparency or optical properties.
- Reduced Impact Resistance: Prolonged exposure to extreme conditions during sterilization can reduce the impact resistance of polycarbonate. This may result in a decrease in the material’s ability to withstand mechanical stress or impact, potentially leading to structural failure.
- Loss of Mechanical Strength: Polycarbonate can experience a reduction in mechanical strength, such as tensile strength or flexural strength, when exposed to conditions that exceed its tolerance. This loss of strength can compromise the functionality and safety of components made from polycarbonate.

Figure #1 Distal tip of a colonoscope with a scratched and cloudy lens

Figure #2 Scratched and crazed lens
For endoscopes, there are better lens solutions than polycarbonate
Synthetic sapphire and Lexan (a brand name for polycarbonate) are both materials with distinct characteristics, and their suitability for use in endoscopes depends on various factors. We compare the performance characteristics of synthetic sapphire and Lexan when used for endoscope applications:
- Optical Clarity:
Synthetic Sapphire: Synthetic sapphire has excellent optical clarity and high light transmittance in the visible and near-infrared (NIR) spectra. It can provide clear, high-resolution images with minimal distortion.
Lexan: Lexan also has good optical clarity, but it may not match the optical quality of synthetic sapphire. Polycarbonate can exhibit more optical distortion, particularly in thinner sections.
- Durability and Resistance:
Synthetic Sapphire: Sapphire is extremely hard and scratch-resistant, making it highly durable. It can withstand abrasive environments and maintain its optical clarity over time.
Lexan: Lexan is durable and impact-resistant, but it is not as hard as sapphire. While it can resist impact and some scratches, it is more susceptible to surface damage compared to sapphire.
- Weight:
Synthetic Sapphire: Sapphire is relatively dense and heavier than polycarbonate. This weight difference may be a consideration, especially in endoscopes where weight reduction is essential. Some of the weight concerns be alleviated by the thickness of the material chosen.
Lexan: Polycarbonate is lightweight and can help reduce the overall weight of an endoscope, which can be an advantage for handheld or portable devices.
- Flexibility:
Synthetic Sapphire: Sapphire is rigid and does not flex or bend. It is typically used in rigid endoscopes, where flexibility is not required. Size and design shape of the sapphire can be optimized for use case when added flexibility is required.
Lexan: Lexan is flexible and can be used in the construction of flexible endoscopes, which need to navigate curved paths within the body. Its flexibility allows for better maneuverability in such applications.
- Thermal Properties:
Synthetic Sapphire: Sapphire has excellent thermal stability and can withstand high temperatures without deformation or degradation.
Lexan: Polycarbonate can soften and deform at relatively low temperatures compared to sapphire. It may not be suitable for high-temperature endoscopic procedures.
- Cost:
Synthetic Sapphire: Sapphire is more expensive than polycarbonate, which can significantly impact the cost of manufacturing endoscopes; however, its durability and strength make it an ideal material for endoscope reprocessing and overall lowest total cost of ownership due to its reusability.
Lexan: Lexan is a more cost-effective material choice for endoscopes, especially for disposable or lower-cost devices or when reprocessing is not a planned option.
Endoscopic reprocessing is a crucial aspect of maintaining the safety and effectiveness of endoscopic procedures. Proper reprocessing helps prevent the transmission of infections between patients and ensures that endoscopes are in optimal working condition. However, there are several challenges and potential problems associated with endoscopic reprocessing:
- Inadequate Cleaning: Failure to thoroughly clean the endoscope after each use can lead to the retention of organic material, blood, mucus, or debris. Inadequate cleaning can compromise the effectiveness of subsequent disinfection or sterilization processes.
- Complex Design: Endoscopes have intricate and complex designs with multiple channels, lumens, and components. Ensuring that all areas are properly cleaned and disinfected can be challenging, and incomplete cleaning can pose infection risks.
- Human Error: Endoscope reprocessing requires strict adherence to protocols and guidelines. Human error, such as incorrect handling or improper cleaning techniques, can lead to reprocessing failures.
- Biofilm Formation: Microorganisms can form biofilms on the surfaces of endoscope channels and lumens, making them resistant to cleaning and disinfection. Biofilms can act as reservoirs for infectious agents.
As mentioned above, this is where synthetic sapphire lenses outperform polycarbonate and other traditional lens materials. The advantages include exceptional hardness, optical clarity, high temperature resistance, chemical resistance and durability. Figure #3
In summary, the choice between lens materials for endoscope applications depends on the specific requirements of the endoscope, including optical performance, durability, flexibility, and cost considerations. Synthetic sapphire offers superior optical clarity and scratch resistance. Synthetic sapphire should be at the top of a designer lists and the design should align with the intended use and design of the endoscope.










